
As the nation’s first medical school celebrates its 250th anniversary, a look back at how generations of students, faculty, and alumni have served their country, delivered the finest patient care, and advanced medical research and education here in Philadelphia and around the world.
BY DAVE ZEITLIN | Illustration by Ellen Weinstein
Sidebar | Embedded Education

In its long history, many traditions have been born at the University’s Perelman School of Medicine. But Dean J. Larry Jameson’s favorite is a simple one that began only recently.
For many years at Commencement, a member of the 50th Reunion class has been invited to speak to the graduating medical-school class. But since 2012 a new wrinkle has been added: at the end of these remarks, the speaker asks their classmates in the audience to reach out their hands to symbolically welcome the new class into the profession of medicine.
“At that moment, you really have a 100-year span of time,” says Jameson, who is also Penn’s executive vice president for the health system. “You have people who have been in practice for 50 years reaching out to a graduating class that will practice for the next 50. It’s a remarkable way to understand the link between the alumni and the students and the span of time they’ll share together.”
That connection was on full display at the medical school’s celebration of its 250th anniversary over Alumni Weekend in May, which included panels featuring prominent alumni, a ribbon-cutting to unveil a state-of-the-art medical education center, and a black-tie gala on the steps of the Philadelphia Museum of Art featuring an epic fireworks display.
About 36 hours before the fireworks went off, members of the Class of 1965 kicked off the weekend with a far more low-key—but perhaps even more awe-inspiring—discussion about all that’s changed in the world of medicine since they graduated from Penn a half-century ago.
R. Barrett Noone M’65 GM’71 GM’73 gave the subject a vivid personal twist when he quizzed the audience on who among them had received a string of diagnoses and procedures that included sleep apnea, laparoscopic surgery, a coronary artery stent, and an implantable cardiac pacemaker. As scattered hands went up for each example he gave, the plastic surgeon then asked which of them had experienced all of the above, and was still practicing medicine—to which he raised his own hand.
Nothing he’d mentioned had been discovered or invented in 1965, Noone noted. “I’ve had all of these things and, remarkably, I can still work. That’s what’s happened in medicine in the last 50 years. And who knows what’s going to happen in the next 50 years? It’s really remarkable.”
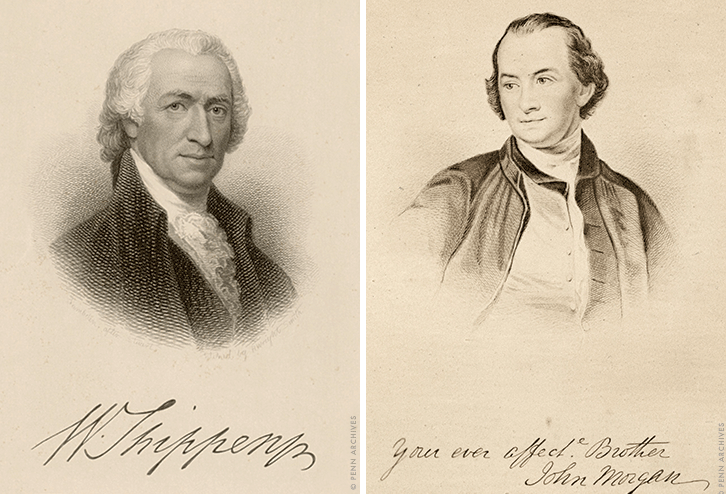
Medical faculty and students have been at the forefront of many advances in patient care and research since the school got its start in 1765, when founder John Morgan and surgeon William Shippen Jr., soon joined by chemistry teacher Benjamin Rush (better known as the “father of psychiatry” [“Rush’s Remedies,” Jul|Aug 2012]), and pharmacology professor Adam Kuhn, began teaching classes at the University. “Fast forward a mere 250 years,” Jameson says, “and we have more than 2,000 faculty.”
Among them have been professors responsible for major medical breakthroughs, ranging from Peter Nowell M’52’s 1960 discovery of the Philadelphia Chromosome—which demonstrated that cancers could be caused by genetic mutation—to the remarkable work of Carl June and his Penn Medicine colleagues to destroy cancer by using a patient’s own re-engineered T-cells [“The T-Cell Warriors,” Mar|Apr 2015]. There have been pioneers like Emily Hartshorne Mudd, a champion of women’s rights and an early marriage-counselor who was the first woman to be named a full professor at the medical school; an Olympic Gold Medalist (biophysics and biochemistry professor Britton Chance C’35 Gr’40 Hon’85); a scientist who published his views on natural selection six years before Charles Darwin released On the Origin of Species (paleontologist Joseph Leidy M1874). Other Penn Medicine notables include the first American physician known to have practiced western medicine in China, James Bradford M1823; and even a major American poet in William Carlos Williams M1906 Hon’54.
But Jameson emphasizes that Penn is not just about the famous innovators and pioneers among the faculty and alumni. It’s about the legions of doctors around the city, country, and world who devote themselves to their profession—and who return to their alma mater and reach out their hands to the next generation of doctors schooled at the same place they were.
“Our alumni are the best representatives that we have for Penn Medicine,” Jameson says. “Wherever they go with their careers, they carry that identity and bring the reputation with them. One of the reasons we’re such a highly regarded medical school is because our alumni have been so successful.”
As an alumnus who also worked with Penn students as the associate dean of student affairs and residency director in the OB/GYN department throughout the 1990s, William Beck M’65 GM’70 understands this connection as well as anyone. That’s why he comes back to Penn every May from his home in Montana. Beck moderated the 50th Reunion panel and led this year’s graduating class in reciting the Hippocratic Oath.
However much medical technology has advanced in the last half-century, the “art of medicine” and the “interaction of the doctor-patient relationship” is as critical now as it was in 1965—or 1765, Beck believes. So when he and the rest of his classmates extended their hands at Commencement, a part of him hoped they could “bequest some of that art” to the graduating class, he says. “It’s essentially the passing of the baton to the next generation of new doctors. There are obviously many years between our class and this class but it represents the transition from one era to another and the continuity of medicine—especially medicine here at Penn.”

Dressed in colonial garb, Howard Eisen M’81 GM’84 weaves his way through a tent between College Hall and Houston Hall, passing a man wearing a similar outfit. It’s Ben Franklin. He’s John Morgan. They exchange pleasantries and move on.
“I get along well with him,” quips Eisen, in character for his role as Morgan during the 250th Penn Medicine Alumni Parade and Picnic. “It was Shippen that was the problem.”
While Eisen—who in daily life is one of the most experienced transplant cardiologists in the world—is familiar with the tension that existed between Morgan and Shippen, the two men most responsible for bringing medical education to the United States, many others are not.
That’s where Clyde Barker comes in.
Barker has been on the medical school faculty since 1966, having served in a variety of capacities, including chairing the Department of Surgery from 1983 to 2001. But lately a lot of his time has been devoted to his unofficial role as Penn Medicine’s historian-in-chief, in which capacity he gave a series of talks to alumni groups leading up to the 250th anniversary.
He usually opens his talks with the story of Morgan and Shippen—onetime friends who both grew up in Philadelphia and got their medical training in Europe, learning anatomy in London and receiving their degrees from the University of Edinburgh in Scotland. After his return, Shippen began teaching anatomy classes in downtown Philadelphia, which Barker calls “the first official lectures that were given in this country in medicine.” When Morgan came home three years later, the two men finalized plans to open a medical school together in Philadelphia. But when Morgan presented the proposal for the Medical School of the College of Philadelphia (as the University was then known) to the trustees, he excluded Shippen. That was a mistake.
“I guess he wanted all the credit to himself,” Barker says. “But Shippen was a very powerful person. His family was one of the first families in Philadelphia.” Morgan also “absolutely denigrated surgeons and anybody who had been trained by the apprenticeship system,” he adds. “That included all of the doctors in the country. So immediately he made an enemy of almost everybody that was around him.”
Morgan was a “visionary,” whose plan for the school “we still admire,” says Barker—largely because it intricately tied the medical school to the broader university rather than choosing a more isolated clinical setting—but he was also the kind of person who had “no knowledge of human nature or any sense of humor.” Those personality traits led to his being dismissed as the chief physician of the Continental Army during the Revolutionary War, a job he took after 10 years of teaching at Penn. His replacement in the post, naturally, was Shippen—which only deepened the enmity between them. According to Barker, Morgan “spent almost 100 percent of his time trying to get back at Shippen” from that point forward. With the help of Founding Father and fellow Penn professor Benjamin Rush, Morgan eventually engineered Shippen’s resignation from the army—but that only brought him back to Penn, where, Barker says, he did much better work, anyway.
While Morgan gets most of the credit for the school’s founding, in his day he “was not the survivor of the rivalry,” Barker says. After he went off to war, Morgan never again taught at Penn, but “William Shippen, his rival, came back to the school and taught for another 30 years. So the short-lived success of the two was more on Shippen’s side than Morgan’s side.”
Personal squabbles aside, the two men, bound together by history if not friendship, played equally vital roles in laying the foundation for the medical school’s two-and-half centuries of excellence in medical education, research, and patient care. And that’s the message Barker tries to get across when he shares their story.
“Neither one of them can be given a lot of credit for their army time,” he says. “But they made wonderful contributions to Penn—Morgan in terms of his plan for the school and Shippen in terms of having been the strongest teacher in the school for decades, teaching not only anatomy but surgery and midwifery. When he finally retired after 40 years, it took three people to replace him.”
Perhaps it was the costume talking, but Eisen is partial toward Morgan for having the “tenacity” and “courage of his convictions” to do something no one else in this country had done before. “In the New World, establishing a medical school back then was quite an intrepid thing to do,” Eisen says. “John Morgan had the vision. And it happened here. It happened here first.”
Still, he thinks he’ll probably retire the Morgan outfit—at least until the 275th anniversary.
If neither Morgan nor Shippen was particularly effective as director of hospitals for the Continental Army, their service nevertheless began a tradition that compellingly illustrates Penn Medicine’s historic impact. According to local writer and historian Carol Perloff C’80 GFA’84, medical faculty, students, and alumni from Penn have served the United States in every major military conflict since the American Revolution. She describes that work in a chapter of To Spread the Light of Knowledge: 250 Years of the Nation’s First Medical School, a book she wrote with help from Penn Medicine’s communications department and the University Archives and Records Center (which can be ordered online at bit.ly/PSOM250).
“Every time I came up with another person who served at a very high level, I’d find more,” Perloff says. “Penn really made a huge impact in the major wars this nation’s fought. That’s who was out there.”
Members of Penn’s faculty and at least 40 medical alumni, including all but one member of the Class of 1778, joined Morgan and Shippen in the fight for American independence. Another early medical graduate, David Hosack M1790, was the attending physician for Alexander Hamilton at the famous 1804 duel in which Aaron Burr shot and mortally wounded Hamilton. Eleven years earlier, many Penn faculty members and their apprentices were in the trenches treating victims of Philadelphia’s 1793 Yellow Fever epidemic, some of them dying for their efforts.
More than 1,000 medical alumni and students served in the Civil War, with nearly half representing the Confederacy, since Penn had attracted many students from below the Mason-Dixon Line [“Penn Fights the Civil War,” Mar|Apr 2011]. “No other medical school in the country supplied as many physicians in the field as we did during the Civil War,” says Mark Frazier Lloyd, the director of the University Archives and Record Center. “That is muted here in Philadelphia because many of the physicians served in the Confederate Army, not the Union. Nobody in the North likes to brag about how many military officers in the Confederacy they educated.”
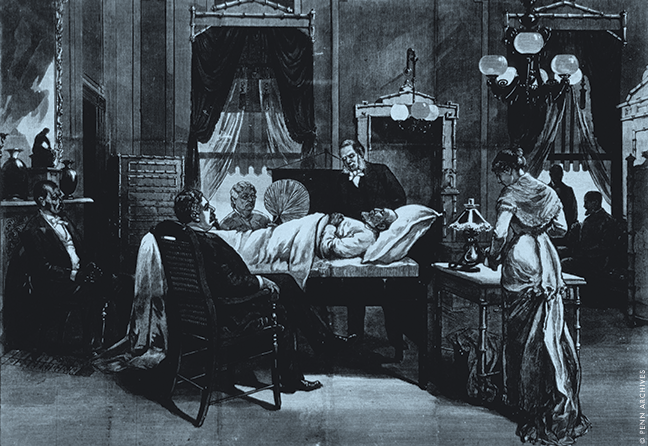
Perhaps the most prominent alumnus of the Civil War era was Joseph Barnes M1838, who was the Surgeon General of the United States Army from 1864 to 1882. Most famously, Barnes attended President Abraham Lincoln on his deathbed, as depicted in an 1865 lithograph. Along with longtime Penn faculty member D. Hayes Agnew M1838 (himself immortalized in Thomas Eakins’ The Agnew Clinic), Barnes was also one of the surgeons who tried to save President James Garfield after he was shot on July 2, 1881; Garfield died two-and-a-half months later.

Penn’s service continued during World War I and World War II. In the former conflict, 40 percent of the medical faculty enlisted in the armed forces by June 1917, including Dean William Pepper III M1897. (All told, Pepper served as dean from 1912 to 1945. His father, William Pepper Jr. C1862 M1864, was also a longtime faculty member—credited with opening the Hospital of the University of Pennsylvania in 1874—and served as Penn’s provost from 1881 to 1895.)

Penn doctors staffed base hospitals during both wars, with surgeon I.S. (Isadore Schwaner) Ravdin M1918 running the 20th General Hospital, near the India-Burma border, in World War II. According to Barker, HUP essentially cleared out, with everyone following Ravdin to war.
“Next to William Pepper [Jr.], I think Ravdin was probably the most important person in the history of this school,” Barker says. “Under his command in India was virtually every young doctor who would become a chairman of a department after the war.”
Shortly after he returned from military service, Ravdin was named to chair Penn’s surgery department. That was a tremendous breakthrough in its time, because Ravdin was Jewish. According to Lloyd, “no one ever thought that a Jew could be named the head of the department of surgery.”
Ravdin essentially ran HUP like he did the 20th General Hospital, Barker says. He had his general’s flag by his desk and Barker remembers, as a young intern, seeing the dean of the medical school sitting in a chair outside Ravdin’s office, waiting for an audience.
“He was, without question, the superstar of the medical school in the first half of the 20th century,” Lloyd says of Ravdin, who went on to become a vice president of the University and has a HUP wing named after him. And Barker calls him “undoubtedly the most famous doctor in America at the time.”
Because the same doctors who served under him in the war were also working for him back at Penn, it led to a “very cohesive faculty—and I think that was really the genesis of the coordinated faculty that we have here today in all different departments,” Barker adds. Even more important, Ravdin helped institute and coordinate Penn’s first real residency program and postgraduate training in specialty fields for medical students.
“Then, for the first time, this hospital and departments in the school began to turn out leaders in American medicine,” Barker says. “Up until that time, the chairmen in departments of this medical school and chiefs of services in the hospital really acquired those positions by succession—sort of like English royalty.”
One of Penn Medicine’s leaders in the second half of the 20th century served as a colonel at the Army hospital in India during World War II but was not a surgeon like Ravdin. Instead, Francis C. Wood M’26 GM’30 Hon’71 decided to be an internist—so he’d spend less time “washing his hands,” his son Lawrence Wood M’61 GM’65 told a Philadelphia Inquirer reporter for his father’s 1990 obituary. Whatever the reason, the decision was a wise one, as Wood’s research led to important advances in the treatment of heart disease, while the medical residency program he directed as chair of Penn’s Department of Medicine from 1947 until 1964 produced many thought leaders in medical education.
Near the end of a discussion of his dad’s contributions as a Penn faculty member at the 250th celebration, Wood read something his father had once written, hoping it would show the humanistic ideals that Francis Wood passed along to so many students at Penn—and to him: “I despise hearing someone say he handles patients well. You don’t handle people; you handle yourself. That is, to me, the crux of the art of medicine. You learn to handle yourself and the patient will respond.”
David Apple M’62 has a vivid memory of his late classmate Henry A. Jordan M’62 GM’67 from when they were both second-year medical students. In pathology class, they were learning how to draw blood in pairs; Jordan eagerly volunteered to go first and stick a needle in Apple’s arm. It didn’t go very well.
“All of a sudden, his eyes rolled back and he fainted and fell on the floor,” Apple recalls. “I think that was the first inkling Henry had that he was not going to be a surgeon.”
Instead, Jordan—whose parents both graduated from the medical school in 1929—became a psychiatrist, as well as an author, wood carver, philanthropist, and the chair of many boards and committees, especially at Penn. In addition to his support for what would become the new Henry A. Jordan Medical Education Center (see sidebar), his many contributions include the Jordan Center for Gynecologic Cancer at the Abramson Cancer Center and the Jordan Family Challenge Fund, designed to encourage others to match his and his wife’s extensive scholarship support. Jordan also served on the executive committee of the Penn Medicine board of trustees, chaired the school’s Campaign for Medicine, and before his death in 2010 was a co-chair of the University’s Making History campaign, not to mention serving as class agent for the Class of 1962.
“If there’s [such a thing as] Quaker blood, I’m sure it was circulating through his veins,” says Apple, who has taken over the class agent role. “That was his number one interest. He kept our class together. He talked to all of us and let us know when we weren’t doing enough for Penn—in a nice way.”
Apple—who in 1975 founded the Shepherd Center, a private hospital in Atlanta that specializes in treatment, research, and rehabilitation for people with spinal cord and brain injuries—was not surprised that his former classmate devoted so much of his life to Penn. For him, the medical school inspired that kind of lifelong support because it was clear from the start that the “professors had an attitude that they weren’t trying to flunk you out—they were trying to make sure you were good doctors.”
Arlene Bennett Ed’60 M’64 shares that feeling. She remembers hearing that students at other medical schools were told things like, “Look at the person on your left, look at the person on your right—some of you will not graduate.” That kind of fear-inducing message was never imparted at Penn. Which may have been especially welcome for Bennett—the first African-American woman to attend Penn’s medical school.
Not that she gave much thought to the distinction back then.
“Now I’m 81 years old, and I look back and say, ‘Wow, that was really something.’ But it wasn’t prominent in my mind at the time, ” says Bennett, a psychiatrist and lifelong Philadelphian. “None of us paid attention. We just wanted to know when the next exam was and what was going to be on it.”
Before coming to Penn as an undergraduate, Bennett had experienced bigotry. While serving in the US Air Force from 1953 to 1956, which she did so she could use the GI Bill for college, Bennett remembers going into a drugstore in uniform to buy a Coke, only to be told by the clerk, “We don’t serve your kind here.”
She also remembers a couple of guidance counselors at the Philadelphia High School for Girls trying to steer her away from a career in medicine. That wasn’t much of a deterrent for someone who had decided at the age of nine that she wanted to be a doctor—in part because of her proximity to the old West Philadelphia Hospital for Women.
“At that time, I thought that all doctors were women,” she laughs.
“So when the counselor said, ‘Oh, you can’t do that, you’re a Negro, you’re a female, you come from humble backgrounds,’ I thought there was something wrong with him, so I just ignored him,” she says. “I’ve never felt uncomfortable being either the only person of color or the only female. It may have bothered the people around me, but it never bothered me.”
According to Bennett, it didn’t bother her classmates, either, who went to great lengths to be inclusive toward her and the five other women in the Class of 1964. Whether it was burning the midnight oil studying together, heading downtown to buy $1 peanut-gallery seats to performances at the Academy of Music, or getting a cheeseburger at Smokey Joe’s, Bennett always felt a strong sense of camaraderie with her peers. She says she can’t recall suffering any form of discrimination while at Penn (as an undergrad or as a medical student). “We were a team,” she says. “That feeling is still there.”
Bennett remains active at the school, currently serving on the Penn Medical Alumni Advisory Council. At her 50th Reunion last year, she spoke to the Class of 2014—where it pleased her greatly to look out in the crowd and see more than a few young black women. She also received the 2014 Elizabeth Kirk Rose Award for her contributions to fostering the education and careers of women in academic medicine—and has, perhaps reluctantly, come to terms with her status as a trailblazer at Penn Medicine, along with the school’s first African-American graduate Nathan Francis Mossell M1882 (whose experience was much less positive, to say the least) [“A Principled Man,” Nov|Dec 2014], and the first female graduates, Gladys Girardeau M1918 and Alberta Peltz M1918.
“It’s a very good feeling,” Bennett says. “Every student at Penn is part of its history, but I think this special history makes me feel like, ‘OK Arlene, you’ve made your contribution.’ I’m going to be writing my memoirs, because I have a young granddaughter and I want her to know about her Nana. And I want other young ladies to not have doubts about their goals and to know that their dreams can be real.”
A couple of times a day, Larry Jameson leaves his office to walk through campus. Besides being refreshed and energized by the bustle of a thriving university, these walks also serve a greater purpose. Often, the dean is on his way to meet with administrators and faculty members at different schools and departments with which the medical school is partnering.
For Jameson, it’s these collaborations—with the Wharton School, the School of Engineering and Applied Science, and others—that set Penn apart from other medical schools in the country. And he believes that collegial spirit has been one of the most important components of its long success.
“The enduring features will be the concept that the field of medicine should be built on a foundation of science, and that the foundation of science is best created and perpetuated by being strongly tied to a university setting,” says Jameson. “There was an option for the medical school to be in a hospital without a tie to the University, and part of our history was the decision not to do that. That feature was turned down, and the proposal by John Morgan to be tied to the University was accepted.”
Among current projects, Jameson cites work with Wharton’s Leonard Davis Institute of Health Economics on a study to incentivize modified healthcare behavior, which he called “a huge problem in medicine that physicians alone have not been able to solve.” The school’s multiple partnerships with the engineering school have been vital, since “our ability to diagnose disease is so tied to technological advances” such as MRIs and CT scans, he says.
“There are other universities that put together these kinds of combinations in different ways,” Jameson adds. “But there are very few, if any, that have a school of medicine, nursing, dental, arts and sciences, business, and engineering all in one geographic location. I do think it’s very unusual to have the diversity of the schools and the geographic proximity that we have at Penn.”
It’s these partnerships, as well as the school’s impressive history, that led renowned trauma surgeon C. William Schwab to first accept a faculty position at Penn back in 1987. “One of the wonderful things about the University of Pennsylvania is we’re all on one campus with the exception of large-animal veterinary medicine,” Schwab says. “It’s very easy to not only communicate but communicate in person. That’s a tremendous asset here. It just makes the experience so much richer.”
Back in the 1990s, Schwab led a public-health study on firearm safety, one of the collaborative research projects he’s most proud of. (“It’s funny, physicians work constantly to put ourselves out of business,” he says.) He first went to a Wharton actuarial scientist to calculate the risk associated with having a gun in a household, then to the engineering school to see if they could make guns and body armor safer. Finally, he worked with experts in other schools to look at the sociological side in an attempt to identify those people who may do harm to themselves (like the elderly or depressed) so it could be reported to their healthcare providers. The feedback on the study, he said, was excellent.
“It was very interdisciplinary, even transdisciplinary, to try to find out ways of preventing gun injury before it occurred,” he says. “Not all institutions can take on something like that with the magnitude, depth, and breadth of the University of Pennsylvania. That’s one of the things that always attracted me and really made me want to stay here and continue to serve on the faculty.”
Schwab has just completed what he calls “the most daunting and complex project I’ve ever done in my life”—the opening of the University’s new Trauma Center at Penn Presbyterian Medical Center [“Gazetteer,” May|June]. The transition of Penn Medicine’s Level 1 Trauma Center from HUP to Penn Presbyterian across campus in February marked the continued evolution of Penn’s commitment to caring for the severely injured, says Schwab. That commitment goes back through the nation’s armed conflicts and continuing into the 1970s, when Penn people like former surgery department head Jonathan Rhoads GrM’40 Hon’60 were “very prominent” voices calling for “trauma centers, trauma systems, and trauma surgeons.” The new trauma unit will continue to serve as a vital training ground for students, who need to learn how to make rapid decisions if they want to go into emergency care.
“We built it large enough for education, so it’s equipped so that people can have a great clinical experience and then we can debrief and meet in a conference room and teach one another about what that experience was,” Schwab says. “It’s an integrated, collaborative teaching hospital. And we built research space. To me, it’s the ultimate fulfillment of the tripartite mission of academia: great clinical care, wonderful education, and phenomenal research.”
With the new trauma center and the Jordan Center among the facilities opening this year alone, it’s no wonder Jameson says that “if you want to be a leader in academic medicine, this is the best place to be in the world.” At the same time, the dean doesn’t like to thump his chest about the Perelman School’s virtues because that could negate all of the partnerships it’s worked so hard to foster.
“Excellence permeates Penn Medicine, but I think we do it without being arrogant,” Jameson says. “And that’s no small statement, because if you achieve excellence and it’s coupled with arrogance, it can make it very difficult to have a warm collaborative community. I think the collaborative environment at Penn is a very strong value that’s been there for a long time.”
Edward J. Stemmler M’60 sits inside the brand new Law Auditorium in the Jordan Center, his cane resting on the desk in front of him. Soon, his lips begin to quiver and tears well in his eyes. Sitting in front of him and speaking during an alumni panel is Patricia Gabow M’69 GM’73, who before emerging as a national leader for hospital reform as the CEO of Denver Health was an unsure medical student—until she met Stemmler, a former dean who worked at Penn from 1964 to 1990.
“He was incredibly supportive to me,” Gabow says. “I remember one encounter where I went to him for some advice, and I wasn’t up to the task. He said to me, ‘Patty, the cream always rises to the top.’ I didn’t think I was the cream, but it was important that someone thought that.”
A few hours later, as he sits inside a tent during the alumni picnic, Stemmler is still emotional as he thinks about Gabow and all of the other students he helped to find their way.
“She was a star as a student and, typical of Penn, when she went away, she continued to be a star,” says the 86-year-old Stemmler, the school’s oldest living former dean. “There were so many people when I was there who are now doing wonderful things, and that’s what being a dean is all about. You don’t do these things yourself. You try to help somebody else do them.”
Gabow wasn’t the only one who shared how Penn groomed them for future success. At the 50th reunion panel, psychiatrist Kent Neff M’65 recounted a story about the medical school loaning him $1,000 to buy a used car when his car died just before he was visiting other schools for internships.
Arlene Bennett jokes that she can hardly recognize the medical campus these days—but she still comes back as often as she can. “I think Penn, and certainly the medical school, it grows on you,” she says. “It becomes a part of you. I think for most of us, we can’t help but think of the medical school every day because that’s what we’re doing. We’re doing what they taught us.”
Having a dedicated alumni base—archivist Lloyd contends that the “medical alumni from day one have invested more in their school then comparable alumni have at other institutions”—made it easier for Rosemary Mazanet G’81 M’86 to plan the festivities as the co-chair of the 250th anniversary weekend.
And despite a thunderstorm, the gala went off without a hitch as about 1,200 people packed a beautiful tent outside the Art Museum—“Whoever made the decision about the tent,” Philadelphia Mayor Michael Nutter W’79 deadpanned after coming in from the rain, “thank you”—and dignitaries such as Nutter, journalist Andrea Mitchell CW’67, and Penn president Amy Gutmann addressed the crowd.
In her remarks, Gutmann praised Raymond and Ruth Perelman, whose $225 million gift in 2011 created a permanent endowment for the school, which was then named in their honor. Later, Jameson presented the 2015 Penn Medicine Dean’s Medal to Walter Gamble M’57 and his wife Anne, who together established a scholarship program that’s provided 223 students with full four-year medical scholarships.
“Most alumni have a strong positive relationship to their experiences at Penn Medicine,” says Mazanet, a trustee and former co-chair of the Making History campaign. “So that makes it easy for me to have enthusiasm. Whenever I talk to people, they feed into that. They validate my enthusiasm.”
“I feel like I was enormously fortunate to go to Penn Medicine,” she adds. “And I just want to have other people realize their dreams. I’m very proud of Penn, and I feel compelled to share that.”
Midway through the gala, before Harry Connick Jr. played some jazz music and a choir belted out a song as fireworks popped in the background, Gutmann boasted that no other medical school in the country has alumni that are as “devoted, passionate, and visionary as ours.” And then she added, “Looking over this spectacular crowd tonight, I am confident that the Perelman School’s future will be even more successful for at least another quarter-millennium.”
She’s not alone in her confident outlook. School historian Clyde Barker—a world-renowned transplant surgeon who began the University’s transplant program in 1966—likes to joke with his colleagues that none of them “would have a chance to get into medical school here anymore” because the “students get smarter and smarter.” Which provides plenty of reasons to be optimistic about future life-saving breakthroughs.
“I think there’s a real risk in thinking that everything important has already been discovered,” says Jameson, “because what we continuously learn is that you turn the next corner and there’s some previously unimaginable opportunity that’s before you that you now have the tools to explore further. So I have no doubt that the pace of advances will do nothing but accelerate going forward.”
Whatever those discoveries might be, and however the practice of healthcare changes in the next 50, 100, or 250 years, the dean of the country’s oldest medical school is sure of at least one thing: Penn’s core mission will never stray from its historic ideals.
“Every medical school in every university has its own personality and identity,” Jameson says. “I think the culture here is very focused on: How can we make new discoveries for societal good? How can we deliver healthcare that improves the lives of people regardless of their means?
“It’s largely a reflection of the culture of the institution, and cultures don’t change very fast. In the case of Penn, that’s a good thing.”

Embedded Education
If you want to see the future of medical education at Penn, stand outside the neighboring Perelman Center for Advanced Medicine and the Smilow Center for Translational Research on Civic Center Boulevard—and look up. Perched five stories above ground, at the meeting of the two structures, is the new Henry A. Jordan Medical Education Center, which got its official ribbon-cutting as part of the Perelman School of Medicine’s 250th Anniversary celebration in May.
The Center came about as the result of some out-of-the-box thinking by Gail Morrison M’71 GM’76, Penn Medicine’s senior vice dean for education, and the willing imagination of Barrie Jordan, the widow of Henry Jordan M’62 GM’67, for whom the Center is named. (Jordan, an extraordinarily active and generous Penn Medicine volunteer leader and donor, had pledged support for a new building for medical students before his death in 2010.)
Morrison had been pursuing a new space for medical students almost since revamping the school’s curriculum in 1999, but without ever hitting on the right plan. Eventually, she realized that the ideal spot was on the roof of the recently completed Smilow Center. That location would physically connect the space to both that facility and PCAM, putting it right in the midst of Penn Medicine’s outpatient and research facilities, a short elevator ride away from real patients and on-the-job training, and just across the street from HUP.
Originally, the area was designated to be a green roof, and a roof is what Barrie Jordan saw out the window when Morrison took her up to the fifth floor of the Perelman Center. Then Morrison asked her to close her eyes and imagine that she saw a beautiful glass-enclosed space that would rise up 38 feet in the air and change the way medicine is taught at Penn.
Jordan opened her eyes and smiled.
“On the spot, she literally said, ‘Yes, I agree,’” Morrison recalls.
For Morrison, it’s perfect timing that the completion of the Jordan Center coincided with this milestone in the school’s history. As Penn Medicine celebrates its past, it can also look to the Jordan Center as a beacon of innovation for the future. “This may be the new model,” Morrison says. “It never used to be the model that education got embedded—literally embedded—into the medical center. I hope it’s the new model. Penn does like to lead the way.”
On an early spring afternoon, Morrison has a bounce in her step as she walks through the Jordan Center, where her new administrative office is located. “They call it JMEC,” she laughs, passing some bleary-eyed students, who’ve been able to make use of the facility since February, ahead of the formal opening in May. Already, she’s noticed those students making plans to stay at JMEC even when they don’t have class—exactly what she hoped the double-high ceilings, light-filled classrooms and gorgeous views of the city would inspire.
“Medical schools aren’t the most modern places,” she says. “I think this is saying that learning is very different today than it was 30, 40 years ago. Learning is no longer sitting in a lecture room and just memorizing facts. It’s really working together with people, analyzing situations and working across disciplines. You need a space that’s convenient and makes you feel good. Sometimes we don’t think about that, but being in a place that makes you smile and feel good does help in this whole process. It’s the right space for the right time.”
In addition to the small study-rooms, technology-rich classrooms, larger seminar rooms, computer lab, café, outdoor patio, and student lounge (with a pool table and Ping-Pong table), the Jordan Center is also home to the high-tech Joseph and Loretta Law Auditorium, which has seating capacity for an entire class. Outside the auditorium are another 6,000 square feet of breakout space for receptions, complete with arguably the best view anywhere on campus. “It’s pretty dramatic,” Morrison says as she looks out the window in the direction of HUP.
Brothers Dennis C’69 M’73, Ronald C’71 M’75, Christopher C’78 M’82, and Jeremy M’86 Law gave $3 million for the auditorium, which honors their parents (who participated in the grand opening via Skype from Hong Kong). And the entire Jordan family was on hand at the ribbon cutting in what was an emotional ceremony for one of the school’s most philanthropic alumni.
“If he were here, he’d be smiling,” Morrison says of Jordan. “That much I know.”
Dave Zeitlin C’03 writes frequently and on a variety of subjects for the Gazette.




