
When a Penn-CHOP team performed the world’s first double hand transplant on a child last summer, the landmark operation generated headlines around the world and young Zion Harvey became a YouTube star. But there’s a lot more to the story.
BY DAVE ZEITLIN | Illustration by Chris Gash

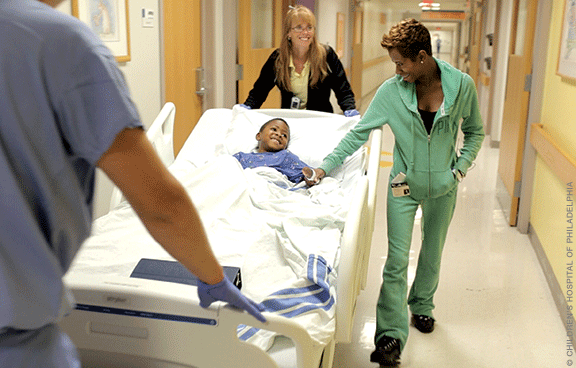
On July 28, the Children’s Hospital of Philadelphia released a video that captivated the world. In the 13-minute inspirational clip, we meet a precocious eight-year-old boy from Baltimore named Zion Harvey, who likes to play foosball, wants to get a puppy, and, at the age of two, lost both of his arms and legs because of a life-threatening infection. He had arrived at CHOP not long before, hoping for new hands but knowing full well that a double hand transplant surgery had never even been attempted on a child. But, as the video shows, he was never fearful.
“When I get these hands, I will be proud of what hands I get,” he says at one point, thumbing through a catalogue of skin colors, before walking over to his mother on his prosthetic legs. “And if it gets messed up, I don’t care. Because I have my family.” Then, he nuzzled right up to her face and they hugged.
“You need like a Hollywood script writer,” CHOP’s surgeon-in-chief N. Scott Adzick would later say. “I mean, it’s unbelievable.”
A young child keeping that kind of perspective (“My grandmother says I’m smarter than a lot of grown-ups,” Zion boasted later in the video) combined with his boyish love for life (the biggest reason he wanted new hands, he told his doctors, was so that he could swing on the monkey bars) is what captured the hearts of so many. It’s also one of the reasons he was chosen to become the recipient of the world’s first pediatric bilateral hand transplant by L. Scott Levin, director of the Hand Transplant Program at CHOP and Penn Medicine, as well as chair of Penn’s orthopaedic surgery department.
“What’s most impressive is that every moment that I’ve cared for him, this little guy has been attentive and communicative,” Levin says. “Not one whimper, not one display of sadness, never withdrawn. It’s as if nothing happened to him. That lifts everyone up.”
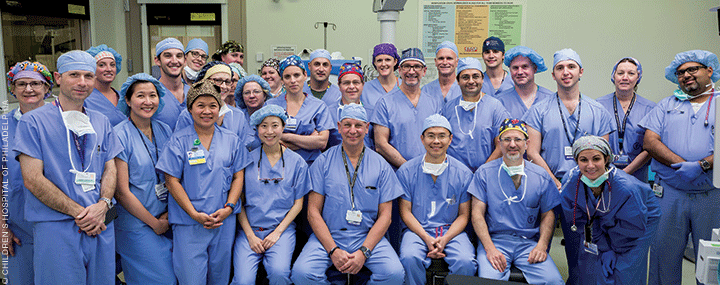
A 40-member multidisciplinary team of surgeons, physicians, nurses, anesthesiologists, and radiologists—led by Levin and Benjamin Chang, co-director of CHOP’s Hand Transplant Program and associate chief of the Division of Plastic Surgery at Penn Medicine—completed the landmark 11-hour surgical transplantation in July.
The operation was a resounding success, and after working all through the night, Levin, Chang, and two other doctors walked down the halls of CHOP, followed by video cameras, to deliver a historic message to Zion’s mother at 4:32 a.m. “We have some good news for you,” Levin told her. “Your little guy has two hands.” Two days later, a groggy Zion was shown smiling and meeting with his doctors. Two weeks after that, he was shown moving his fingers, clutching a tiny sponge and scratching his eyes.
“He’s incredible,” Chang says. “One of the best patients I’ve ever had of any age, honestly. What you see on that video is really how he is.”
The world certainly took notice of the brave young boy. He held a press conference after the surgery with his mother and doctors. He was featured on Good Morning America, NBC Nightly News, and BBC News. He met pop star Nicki Minaj. By early October, CHOP’s video had nearly 700,000 views on YouTube.
But when the cameras stopped rolling is when the real work began for Zion, who was discharged from CHOP in late August and has a long road ahead of him filled with daily hand therapy, follow-up surgeries, and anti-rejection medication. The work will also continue for Levin, Chang, and the rest of Penn’s team, which four years ago performed the region’s first double hand transplant before again making history with Zion’s surgery.
And they plan to continue to lead the charge.
“Nobody Does This Alone”
Abraham Shaked, director of the Penn Transplant Institute, vividly remembers the day six years ago that Levin—who had previously been a professor of orthopaedic and plastic surgery at Duke University School of Medicine—arrived at Penn.
“He came to this office and said, ‘What do you think? I think we should do hand transplants,’” Shaked recalls. “I said, ‘Let’s do it tomorrow.’ And I’m not joking.”
Shaked and Levin, of course, both knew it would take a lot longer than that to implement a strategy and put a team in place to perform the complex surgery of reattaching limbs from a deceased donor, a practice known as Vascularized Composite Allotransplantation (VCA). After all, the first-ever hand transplant was only done 17 years ago, and that patient—a New Zealander named Clint Hallam—ended up requesting that his new hand be amputated, in part because he didn’t follow through on the post-operative drug and physiotherapy required to avoid having his body reject it. According to Levin, that led to “tremendous skepticism” in the field while serving as a cautionary tale as to how well recipients need to be screened psychologically beforehand.
But with the right set of circumstances, the operation has been proven to work. Just a few months after Hallam’s surgery in France, a New Jersey man named Matthew Scott received a new left hand at Louisville, Kentucky’s Jewish Hospital, threw out the first pitch at a Philadelphia Phillies game the next year, and said in a recent interview that the “15 years since then have [been] nothing short of spectacular.” And six years ago, just a couple of months before Levin made his declaration to Shaked, the first double hand transplant was performed in the US, setting the stage for a new group of patients in tremendous need of help.
“The whole field of Vascularized Composite Allotransplantation is here to stay,” Levin says. “It’s not going away.”
Much of Levin’s devotion to the cause stems from his time in the military, where he was a reservist in the first Gulf War and later served as the Orthopaedic Trauma Association’s Landstuhl Scholar, caring for wounded soldiers at the Landstuhl Regional Medical Center in Germany, a staging center for soldiers brought in from Iraq and Afghanistan. But while it’s become a personal mission of his, he also knows what kind of a team effort VCA requires—which is why Shaked’s eager embrace of the hand-transplant program meant so much to him.
“We’ve become almost like brothers,” Levin says of the Transplant Institute chief. “The thing about this is, I established this [program] under the umbrella of the Transplant Institute. That’s where this program lives. This is not a maverick program. This is part of his shop, his fiefdom. And I’m just one of the folks that works in the field of VCA. There’s been no one more supportive or enthusiastic [about] this than Abe Shaked.”
Shaked says the primary role of the Penn Transplant Institute involves oversight—to make sure “all of the regulations are followed,” including how to list patients for organ donations, making sure patient blood is compatible with donors, insuring proper donor consent, and similar issues. And much of that work centers around the Institute’s partnership with the Gift of Life Donor program, a Philadelphia-based nonprofit organ and tissue transplant network.
“When we decided we wanted to help patients through VCA and hand transplant, one of the first calls made was to Gift of Life,” says Stacey Doll, the Institute’s director of transplant quality and regulatory compliance. “We did a lot of work together with them to practice how we would perform a deceased donor recovery and how we could orchestrate and protect the process that needed to occur for a solid organ. It took a lot of repetition and conversation to establish the processes.”
As Levin’s relationship with Shaked, Doll, and their colleagues at the Transplant Institute was growing, the orthopedist also forged what others have described as a perfect partnership with Chang. From the start, the two meshed well, both because they shared the same goal and also because they have very different personalities. CHOP’s Adzick, who oversaw the surgical team there, describes Levin as the natural-born leader who gave “a Knute Rockne pregame speech” before Zion’s surgery, while Chang is the “mild-mannered reporter for a great Metropolitan newspaper who turns into Superman” when he gets into the surgical room.
Comic-book references aside, Chang agrees with this assessment and believes it has been instrumental in the hand-transplant program’s success.
“He’s a very high-energy person,” Chang says of Levin. “And with his position as the chief of a department and being in touch with the dean, the CEO of the hospital—you need someone at that level to drive this forward. My job is being the detail person. He does the big picture. We fit together, and we don’t try to compete and do the same job. Over the years, it’s become clear what I’m good at and what he’s good at, and those two are not the same.”
According to Chang, his plastic-surgery department had planned to start hand transplants even before Levin arrived at Penn. But rather than trying to have his orthopaedic department compete against them—a “natural rivalry” that Chang admitted is not uncommon between specialty fields—Levin instead immediately reached out to work together with plastic surgery.
From there, the team expanded to include psychologists, social workers, physical therapists, pharmacologists, and nurses, as well as other transplant surgeons who normally operate on kidneys and livers.
“Nobody does this alone,” Levin says. “I guess it was my idea to do it but you need strong people. I think our surgical group is very close. We believe in one another and have a great respect for each other’s abilities.
“Ben is a phenomenal hand surgeon,” he adds. “He’s a skilled clinician, a brilliant tactician, a brilliant thinker; and he’s been essential in the planning and execution process and care post-operatively. I can’t do this alone. No one person does this alone.”
Once the team was in place, the next step toward Penn becoming the third medical center in the US to perform a double hand transplant was finding the right recipient. She turned out to be a young woman from Virginia named Lindsay Aronson Ess, whose surgery took place in September 2011 [“Gazetteer,” Jan|Feb 2012].
“The Ability To Control My Own Life”
Every day when she wakes up, Lindsay Aronson Ess brushes her own teeth. She gets dressed, brushes her hair, cooks herself breakfast, and walks her Brittany Spaniel mix. Twice a week, she gets in her car and drives two hours from her house in Richmond, Virginia, to a northern Virginia gym called CrossFit Rubicon. There, she lifts weights, does push-ups, and works out on gymnastic rings.
“Anything I put my mind to,” the 32-year-old says, “I find a way to do it.”
Such a concept once seemed impossible for Lindsay, who needed to have both her hands and feet amputated in 2007 when a major infection took over her body following intestinal surgery. She was grateful to have survived the traumatic ordeal, but desperately missed the life she had envisioned for herself after graduating college. Having to rely on her mother for help with the simplest tasks made her long for her old independence.
Four years after her double hand transplant surgery at the Hospital of the University of Pennsylvania, her nerves have grown into her new hand muscles and she’s performing functions better than anyone at Penn expected.
“Sometimes we get videos of what she can do,” Shaked says. “It’s mind boggling. Lindsay is a great ambassador—not just for Penn but for this procedure.”
It wasn’t easy, of course. For the first two years after the surgery, she went to rehab for several hours every day. The next year, she went three times a week, for two hours a day. Eventually, she got frustrated, and admits she wasn’t “as consistent” with her hand therapy as she should have been. But she’s made up for it by going to the gym daily and joining a competitive CrossFit team with other people who have lost limbs.
They call themselves “Team Some Assembly Required.”
“We’re a very powerful team,” Ess says. “We’re lifting weight that people don’t even lift able-boded. It’s motivational.”
Even more important is the camaraderie she’s built on the team, which she said has “definitely given me a purpose.” Now she’s even learning to coach, so she can “continue to pay it forward and help other adaptive athletes.”
“Besides lifting weights, [the best thing is the] ability to control my own life again,” Ess says. “I think one of the reasons Dr. Levin chose me as a good candidate is because I am hard on myself. And I do try. I try and try and try until I do it. I don’t give up. But I do get very frustrated.”
There are still things she can’t do with her new hands, no matter how hard she tries. When jars are too tight, it’s difficult for her to twist them off. Small buttons cause her problems. So does cutting meat. She can’t put her own hair up.
But when she needs a little bit of help, she can always call her mother over. She also knows she can lean on Levin.
“Dr. Levin is like another father figure for me,” she says. “I can tell him anything. I’m very open with him. He’s very open for me … I don’t even consider him a surgeon. I consider him more like family. He’s definitely one in a million. I have sat with other surgeons in the same field, and it’s not the same.”
For Levin, maintaining a strong relationship with transplant recipients isn’t a luxury but a priority. The surgery itself, he often says, is simply the first step. In many ways, following up with patients while they’re at home to ensure they’re staying on the right track and scheduling follow-up surgeries and appointments at Penn is equally important.
And if maintaining that relationship also helps Ess become the face of Penn’s hand-transplant program and a symbol of hope for Zion Harvey and all the patients who come after her, well, that’s an added bonus.
“I think she’s going to feel a bond to [Zion] and he to her, I hope,” Levin says. “Not because they’re both my patients, but imagine the dynamic. She can look at him and say, ‘Here’s a child that had what I had as an adult.’ And he can look to her and can see what she can do. That, hopefully, will motivate him.”
Ess and Zion were initially scheduled to meet for the first time in September, but it was pushed back until later this fall because she was under the weather. She isn’t sure what it will be like to meet the courageous boy she watched on YouTube but predicts it will be emotional. She says she’ll probably try to keep it light, though, and make some jokes and show off what she can do with her hands. Unless he asks, she may not offer any advice. That could be overwhelming for an eight-year-old. Besides, there will be plenty of time for that. “I definitely feel like he’s someone that’s going to be in my life for my whole life,” she says. “As long as he’ll have me.”

“An Ideal Candidate”
After the success of its 2011 surgery , and having learned valuable lessons from it, the Penn transplant team started looking for its next patient. While they never specifically set out to make history by operating on a child, they did allow that possibility by expanding the search for candidates to pediatric patients, in light of the close partnership between HUP and CHOP and, as Chang says, “how well positioned CHOP is to do complex surgeries.”
The Penn surgeons first heard about Zion when the Baltimore boy went to Philadelphia’s Shriners Hospital for Children to get fitted for better hand prostheses, since his existing ones impeded his functioning worse than not using prostheses at all. Doctors at Shriners reached out to Levin and Chang to see if they would consider him for a transplant.
That was about a year and a half ago, and the Penn team was being very deliberate with their screening process, hoping to find the perfect candidate for what was still a very new and costly procedure. But after careful consideration, they concluded Zion fit the bill.
One key element in their decision was the fact that the boy was already taking immunosuppressant medication because of a kidney transplant when he was four. Normally, doctors weigh the benefits of transplant surgery against the risks associated with that medication, which patients must take to prevent the rejection of transplanted organs. The fact that Zion was already on it eliminated a major concern.
“The thing that made him special, aside from his personality, was he already had a kidney transplant,” says Chang, adding that the boy’s maturity and excellent family support figured strongly into the decision. “That was really what popped him up on our radar. He turned out to be as close to an ideal candidate as we could have found.”
Once Zion was listed for a transplant with the United Network for Organ Sharing (UNOS), there were still many hurdles to clear. Levin and Chang had to create a new hand-transplant program at CHOP, where they worked closely with doctors to have the procedure endorsed from an ethical standpoint. Meanwhile, since Zion is an African-American child, Chang estimated that there were probably only about 15 potential donors across the entire country that would be a right match in terms of skin color and size. The pool was limited even further by the fact that the organ needed to be within a two-to-three hour flight from Philadelphia.
And yet, in what Chang would later call a “shock” to everyone, it took only three months on the wait list for the hands to be procured. One day later, Zion was whisked in from Baltimore and the surgery began, with team members dropping whatever they were doing to be there for the historic operation.
“I think many surgeons had to leave clinics early, had to cancel surgeries, had to cancel surgeries the next day,” says hand-transplantation coordinator Christine McAndrew, who rushed to the hospital while on maternity leave. “It just goes to show the dedication of the entire team. There was a very happy and energetic vibe the entire night.”
Levin later admitted there was a complication in the surgery. About an hour after Zion got to the intensive care unit following the transplant, they had to take him back to the operating room to redo an artery because he lost blood flow in one of his hands. But the OR team members were prepared to handle that, having gathered several times for rehearsals and following a detailed step-by-step playbook that’s needed to connect bones, blood vessels, nerves, muscles, tendons, and skin from the forearm to new hands.
Everyone knew their specific role and everyone remained calm. Perhaps even more remarkable was how calm Zion was, both leading up to the surgery and in the days and weeks after.
“The first time I saw Zion [after the surgery], he was drowsy but he gave me a smile right away and waved his hand,” says McAndrew, who coordinated the eight-year-old’s pre-operative evaluation and now manages his post-operative care, talking to him and his mother on the phone daily. “His mother was shocked. She said, ‘Chrissy, that’s the first time he waved to anyone with that hand.’”
That, of course, was a special moment for McAndrew. But it didn’t match her astonishment when, just a few days later, Zion told her that he would like to talk to other children who need hands to share his story and “let them know it’s going to be OK.”
Like Lindsay Ess, he wants to pay it forward and be an ambassador for hand transplants. He’s also excited to use his gift to accomplish things in his own life he never thought possible.
In the weeks since his surgery, he’s baked cookies and held action figures. In the future, he hopes to play video games and pick up his younger sister, Zoe. He wants to be able to throw a football. And he even told his mom that he can’t wait to give her a massage.
“I predict this guy’s going to be doing something big-time in his life,” Shaked says. “Maybe one of these days, he’ll be a surgeon. Why not?”
Just the Beginning
The day Zion was released from CHOP, doctors, nurses, and other hospital staff threw a pizza party for him. Zion thanked everyone for his new hands, talked to “people that he didn’t know like they were best friends,” Levin says, and even sang a goodbye tune.
But the end of his hospital stay was just the beginning.
For Zion, there will be a lot of hard work to gain a lifetime of motor function in his hands. Meanwhile, medical experts at Penn and around the world will study his case and try to build upon it to help other children, for whom prosthetic hands “are not that good, especially for smaller kids,” Chang says. And the next step, according to CHOP’s Adzick, is figuring out a way to perform the operation on children who aren’t already immunosuppressed, which would open the door to a slew of new potential candidates.
It could also open the door to ethical questions about putting a child on such risky drugs for an operation that is not life saving. But Levin insists that the medical community should be doing everything possible to help people without arms and legs, especially children and wounded veterans.
“If a little child needed a kidney or a heart or a lung to stay alive, we wouldn’t think twice about it,” Levin says. “Those are life-saving organ transplants. What we’re doing is quality-of-life or life-enhancing organ transplants. But I would look at you and ask right now, ‘If I didn’t have arms or legs, what would life be like?’ Are you going to walk out and get out of the room? Are you going to go to the toilet? Are you going to feed yourself? Are you going to drive? Are you going to use your phone?”
Adds Shaked, “You’re getting into the definition of what is life.”
Levin and his team have already pushed the needle forward on perceptions and regulations surrounding reconstructive transplants. In late 2013, the US Department of Health and Human Services ruled that hand and face transplants would be classified the same way as other organs. “We were instrumental in having that come about,” says Levin, who serves as a vice chair on UNOS’ VCA committee. And now that there’s a national regulatory framework in place, Doll notes, organ procurement organizations are starting to ask potential organ donors for hands, as they would a liver or kidney, noting: “They never did that before.”
According to Chang, publicity for hand transplants could also help such donations become more commonplace.
“One of our worries going into this was that people would think about [hands] differently, and that this was a very unusual request,” Chang says. “And it is unusual. But I think now that it’s been in the news a few times, people have in their mind that it’s a standard part of organ donation.”
Still, there are some other significant obstacles for Penn and the small number of US medical centers that are performing hand transplants. For one, the procedure is not yet covered by insurance companies or subsidized by the government (although the Department of Defense and the Department of Veteran Affairs have become more involved in recent years). CHOP paid for Zion’s surgery, which Shaked calls a “mega expense.” Furthermore, none of the surgeons or other team members were paid, making sustainability a big concern moving forward.
“One might wish to say, ‘OK, we’ve done it once. Now let’s do it 20,000 times.’ But it doesn’t work that way,” Shaked says. “You have to remember we’re talking about something new. Penn cannot transplant 100 people. We would go bankrupt. It’s impossible. It’s depleting our resources. But we are doing it because we believe the science and patient care should be advanced.”
Being on the front lines of innovation, Penn will be in a good position to do more once the procedure is accepted by insurance companies.
Adzick expects that to happen. He compares the emerging field to fetal surgery, which he helped pioneer nearly 20 years ago and which has since corrected debilitating or life-threatening birth defects on more than 1,000 babies still in the womb under CHOP’s Center for Fetal Diagnosis and Treatment.
“We here at CHOP are all-in to support these patients,” Adzick says. “We’re all about innovation and we’re all about caring for children. I don’t worry too much about the financial stuff. We fought this with our fetal surgery work, which initially insurance would not pay for. And now insurance companies nationwide do pay for it.” Hand-transplant surgery is similar “in terms of surgical innovation,” he adds. “And I think this team is going to push things forward on a worldwide basis.”
“I know that Penn will be a leader,” Shaked adds. “This is the place where things are going to be advanced. I don’t have any question about it.”
Because the surgery is still so new and complex, Chang predicts that Penn and CHOP will be one of only about six regional centers across the country where it is done, at least in the short term, which will make it possible to “learn and get better from each operation rather than have it spread across multiple different hospitals where everyone is doing it for the first time.”
Still, the timeline between surgeries likely won’t change much for now. According to Levin, in the wake of the publicity about Zion, there have been 250 inquires from around the world from parents whose children have limb absence or deficiencies. But the screening process will remain as rigorous as ever to ensure not only the best possible recipients but also the best possible care. And finding a suitable donor once patients are listed will still take time.
Penn’s first-ever double hand-transplant recipient thinks often about the growth of the field and what it would mean to so many people like her. But Ess is also concerned that “it’s going to be quantity over quality” at some places and that a “celebrity surgeon” will try to take on the cause.
After four years of constant rehab, and with much more ahead, she knows firsthand that’s not the way to go.
“It’s given me such a better quality of life,” Ess says. “I feel like Penn is the best place to go for hand transplantation. There have been many people who have reached out to me who have had limb loss, and I send them to Penn. To me, it’s the best place not only because of the care I receive but because of my relationship with Dr. Levin.”
And not a day goes by where she doesn’t think about what Levin did for her. Even more than that, she thinks always of the deceased donor who made her new life possible.
“When I look down at my hands, it’s a reminder of the gift,” she says. “I always see them as a gift. They’re not mine. They’re ours.”
Dave Zeitlin C’03 writes on a variety of subjects for the Gazette.




